TOWARDS A D3G GUIDE FOR GRADING MOLAR HYPOMIN
As noted here, D3G aims to develop guidelines that are both clinically useful and research friendly. Collaborative input is sought from the practitioner community, so please let us know what you think as the nascent ideas take shape. If you haven't already done so, please check out our sections on Terminology and Diagnosis before dipping in to Grading here.
The Basics
Here we focus on basic questions, as might be asked by oral health practitioners (hygienists, dental & oral health therapists), dental students and other newcomers to the challenges of managing Hypomin. Hopefully we can work towards formulating reasonably "black and white" answers in this section, and refer remaining "grey areas" onto the specialists. 
Q1: What are the important things to consider when grading Molar Hypomin?
- case level – considering the whole mouth & individual, is this a serious case or not?
- tooth level – are there any severely-affected teeth? – this may be highly influential
- pain level – not necessarily related to severity and again highly influential
Q2: So is this a severe, moderate or mild case of Molar Hypomin?
- severe case – one or more severely-affected teeth
- moderate case – one or more moderately-affected teeth, or a mild case with significant pain
- mild case – one or more mildly-affected teeth
- see examples here (Help needed: please send us any great images you have for here)
Q3: What defines a severely-affected tooth?
- surface breakdown – demarcated opacity with a broken surface (critical feature is visible pitting or degradation)
- typical colour – stronger yellow/brown tones (not critical to grading)
- see examples here (Help needed: please send us any great images you have for here)
Q4: What defines a moderately-affected tooth?
- frosted surface – textured but unpitted opacity, unlike shiny normal enamel (critical feature)
- typical colour – creamy tones (not critical)
- see examples here (Help needed: please send us any great images you have for here)
Q5: What defines a mildly-affected tooth?
- shiny surface – opacity with intact, shiny-enamel surface (critical feature)
- typical colour – bright white, contrasting with less-white normal enamel (not critical)
- see examples here (Help needed: please send us any great images you have for here)
Q6: When is pain considered significant?
- interferes with oral hygiene – localised to affected tooth/region
- interferes with quality-of-life perceptions – including anxiety about dental treatment
Q7: What about caries?
- remember!! – decay/caries in Hypomin enamel is not the same as caries in normal enamel
- is caries consequential to Hypomin? – if clearly yes, this is a useful measure of progression
- so Hypomin has progressed to caries? – useful to know about, both at case and tooth levels
- what is the caries context? – do the "non-Hypomin" teeth have caries?, oral hygiene status?
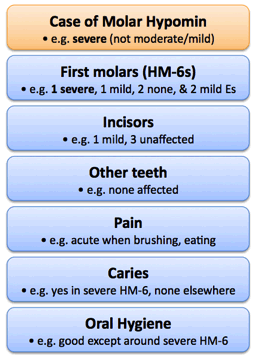 Q8: How might I report a typical case of Molar Hypomin?
Q8: How might I report a typical case of Molar Hypomin?
A basic report might cover case grade, affected/unaffected teeth, pain & caries/hygiene.
For example:
- this appears to be (or is) a classic case of severe Molar Hypomin in an 8-year old
- two 6-year molars are affected severely, one moderately, and one is unaffected (specify teeth)
- two central incisors are mildly affected (specify teeth)
- all other teeth lack Hypomin lesions
- there is chronic pain posteriorly, which the patient finds very disturbing
- one severe molar has progressed to carious dentine, the other lacks visible caries
- otherwise the mouth is caries-free
- oral hygiene is excellent except around the severely-affected molars (pain related)

