Frequently asked Questions (FAQs)

Molar Hypomin ("chalky molars") is a complex subject and so it comes as no surprise that there are more good questions than one can shake a stick at. Here we've tried to cover those that crop up most often. If you've got a question that’s not answered here then let us know and we'll do our best to answer it (contact us).
- Is it my fault that our child has Molar Hypomin?
- How common is Molar Hypomin?
- What causes Molar Hypomin?
- Why these teeth and not others?
- Will the problem pass on to my kid's children?
- How is Molar Hypomin diagnosed?
- Is Molar Hypomin expensive to fix?
- Can Molar Hypomin be prevented ?
- Why do Molar Hypomin teeth hurt?
- Is Molar Hypomin different from decay?
Is it my fault that our child has Molar Hypomin?

No, not at all, and neither is it your child's fault. We do not know enough about what causes Molar Hypomin to recommend anything that families might do to avoid it other than look after your general health as best you can. Obviously it can be particularly frustrating to know that within your family one kid has the problem and another doesn't – but again, you should not blame yourself that maybe you did something wrong to cause this situation. At this stage all we can say is "it's just bad luck, Sam" (read our kids' story about Sam).
How common is Molar Hypomin?
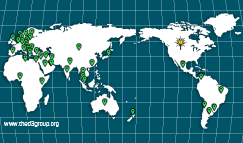
Unfortunately, Molar Hypomin is very common all around the world. A rolling average from over 140 studies shows that about 1-in-5 kids have their 2-year and/or 6-year molars affected to some extent (see a worldwide distribution map and read more about prevalence here). This means that school classes typically may have 4 or 5 kids affected. Thinking about what this means for kids around the world, it seems likely that well over 14 million kids a year get Molar Hypomin worldwide (read more about global incidence of Molar Hypomin), making this a serious and costly problem for public health.
What causes Molar Hypomin?

Research has produced lots of hints that the problem isn't primarily genetic and instead has something to do with illness in infants – in other words, health disruptions (affecting the whole body) somehow damage the developing tooth. But we still don't know whether it’s the illness itself or perhaps the medicines used to treat the illness that’s to blame. It’s also a mystery why some molars can escape "scot free" while others in the same mouth get clobbered, but scientists in Melbourne think they've sniffed out a useful clue about this enigma (breakthrough science). All studies point to the cause being complex so it seems likely that several things must act together to cause Molar Hypomin, rather than there being just one nasty culprit. Clearly, there is a strong need for more research in this area.
Why these teeth and not others?

Research points to it largely being a question of timing. The teeth that end up being affected most often (2-year molars, 6-year molars, adult front teeth) are all pretty much at the same stage of their development in an infant (say from birth to 1-year-old). Conversely, all the other teeth that tend not to get clobbered have either already travelled further down the developmental pathway at that age, or have yet to get that far. So the problem seems to boil down to there being a cause that happens at a certain time (i.e. illness in infants) and, at the same time, some teeth that are at a particular stage in their development which makes them prone to being damaged. Again, there is a clear need for more research on this topic.
Will the problem pass on to my kid's children?

Current research has produced no suggestion that Molar Hypomin has a strong genetic foundation. Most notably, twin studies reveal little difference in Molar Hypomin occurrences (concordance) between identical and nonidentical twins. So, in contrast to another D3 called AI, there is no concern about it being passed on down the family tree. And whilst youngies might be forgiven for referring to their Hypomin teeth as "mutant", this is not the case technically speaking.
How is Molar Hypomin diagnosed?

Dental professionals will look at the appearance of the affected teeth and the number of affected teeth, as outlined here (WHAT DOES IT LOOK LIKE?). They might also assess sensitivity of the tooth by blowing air or spraying water on it. In many cases, and particularly those made worse by dental decay, "X-rays" (dental radiographs) may be taken to assess the extent of damage.
Is Molar Hypomin expensive to fix?

Unfortunately, Molar Hypomin can be expensive to treat in some cases. The particular cost depends on how many teeth are affected and how severe the Hypomin is. It is best to listen to the treatment options that your Dentist explains to you and weigh up the advantages and disadvantages of each. When considering the full costs of treatment, you should ask not only about the immediate costs but also those that may be necessary down the track. Quite commonly, Molar Hypomin needs ongoing treatment into adolescence and adulthood.
Can Molar Hypomin be prevented?

Not yet, but we are hopeful that this desirable situation will come about in the not-too-distant future. First we need to figure out what goes wrong in Molar Hypomin and why – that is, understanding the pathogenesis of chalky enamel and its cause. D3G scientists have recently obtained exciting new clues about this enigma but more research needs to be done (breakthrough science). It's likely that once the cause is known there may be potential to reduce the number of people affected by Molar Hypomin as well as its severity (read more). By supporting Molar Hypomin research you can be a part of D3G's effort to benefit future generations.
Why do Hypomin teeth hurt?

In many cases, Hypomin teeth are soft and porous (chalky) and may even start to crumble away during chewing and cleaning (i.e. "break down"). As a result, the sensitive part of the tooth (dentine) may become exposed and react painfully with things such as cold air, hot foods and drinks, or even just toothbrushing. Most treatment for Molar Hypomin aims to cover up the defective areas, thereby protecting against pain, further breakdown and decay.
Is Molar Hypomin different from dental caries?
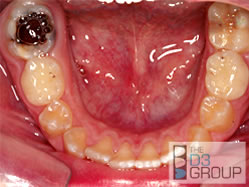
Yes, Molar Hypomin is really very different from dental caries, but it's common for both problems to co-exist in which case "tooth decay" is an appropriate term to use. Conventionally, dental caries happens when normal tooth enamel is attacked by acids, which are produced by sugar-loving bugs in dental plaque. This acid-attack, which can be aggravated by acidic food and drinks, leads to softening of the enamel and subsequently a cavity may form. Unsurprisingly, in Hypomin teeth (which are already soft and porous), the acid-attack can progress extremely rapidly. In contrast to decay, which only affects teeth that have erupted into the mouth, Hypomin first happens when the tooth is developing within the child's jaw – its cause has nothing to do with sugar and plaque. Once erupted, Hypomin teeth may start to crumble even without
excess sugars or acids in the diet. It's particularly important that Hypomin
teeth are looked after carefully to avoid problems with decay.