RESEARCHING FOR BETTER MANAGEMENT AND PREVENTION

Given Molar Hypomineralisation appears to be an acquired disorder, there is good reason to believe it will become preventable medically once the causes are known (read more). Thus a global need exists to learn more about where and when Molar Hypomineralisation occurs (i.e. epidemiology) with a view to finding clues about causation. Allied questions relate to the social and economic costs associated with this prevalent condition (disease burden), which stand as drivers for research funding. Laboratory studies, both basic and applied, are needed to characterise the properties of affected teeth and to investigate how these developmental defects came about (i.e. pathology). Fourthly, a major need "right here and now" is to improve the current management of Molar Hypomineralisation, noting some dental treatments suffer a high failure rate and general absence of bespoke public health policy. Urgent research questions within these four areas are outlined below.
To build a strong and cohesive research capability, The D3 Group has brought together international experts from across the medical and dental science sector (i.e. practitioners, scientists, public health, industry) – see International Friends of D3G and Toronto D3 Symposia.

Together with our Australasian home base (D3G Down Under), this worldwide network provides an unprecedented opportunity to tackle "the Molar Hypomin problem" at global and grass-roots levels.
Today, funding for Molar Hypomineralisation research is very limited due in large part to a general underappreciation of the social and economic costs that this condition imposes on humanity. As always, quality research is expensive yet it seems reasonable to expect that research-centric collectives such as D3G will provide for strong efficiencies when converting research funds into better practice, policy and products – and ultimately, medical prevention (i.e. social good).
EPIDEMIOLOGY QUESTIONS
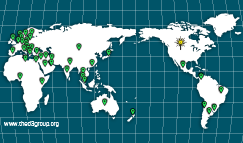
Prevalence data for Molar Hypomineralisation remains rather patchy, despite over 141 studies in 47 countries, raising questions about how bad the problem is in unstudied societies and reasons for inconsistencies evident among existing data. Notable deficits exist both for well-developed populations (e.g. North America) and those less so. Another question is whether Molar Hypomineralisation is on the increase – many clinicians say yes, but on the other hand it could just reflect their increasing awareness of the problem. A pressing need exists to address these and related questions using improved, globally-standardised approaches – see our "Toronto D3 Symposia" for great progress on this front.
COST QUESTIONS
Costs of Molar Hypomineralisation can be identified at multiple levels including affected families (treatments, quality of life), dental practitioners (failed treatments), medical profession (dental emergencies) and the taxpayer come public health system (e.g. hospital services including general anaesthetics). There are many reasons to expect these costs are substantial if not massive, but hard data are generally lacking and so the globalised case for research funding isn't as strong as it should be.
PATHOPHYSIOLOGY QUESTIONS

By analogy to dental fluorosis (where dental hypomineralisation is "acquired" from a known nutritional cause – i.e. overexposure to fluoride), the most pressing question for our field is "what causes Molar Hypomineralisation?". If that tough nut can be cracked then it seems likely this global health problem could become largely preventable, as for dental fluorosis. To pursue such preventive goals we need to filter out the key contenders from the myriad of candidates that have been suggested to play a causal role (e.g. medicines, vaccines, illnesses, fevers and genetic contributions etc). (read more) We also need to better understand how the "chalky enamel" defects actually happen during development (i.e. their pathogenesis), as that too should give clues about cause and avenues for medical prevention – see our recent breakthrough publications here. To tackle these crucial questions, scientists from a range of disciplines need to be engaged (e.g. toxicologists, biochemists, pathologists and biophysical scientists).
MANAGEMENT QUESTIONS
Dental clinicians have many questions about how best to manage the various manifestations of Molar Hypomineralisation – many of their uncertainties concern how best to use existing clinical approaches and dental materials, and others relate to inadequacies of the status quo (e.g. dental materials are routinely optimised for use on normal enamel, not hypomineralised enamel). Research is also needed to guide development of chairside aids that help clinicians (medical and dental) with the diagnosis and characterisation of D3s.
For public health practitioners, management questions extend from community clinics into public health policy and its implementation. Indeed, primary questions may surround difficulties in getting their Molar Hypomineralisation concerns heard, raising need for engagement with the implementation research sector. See here for some great progress on this front Down Under.

