COMMON TREATMENTS FOR MOLAR HYPOMIN
 The way that dental professionals manage Molar Hypomin really depends on how badly your child’s teeth are affected. Of course teeth that are mildly defective require easier treatments than those that are moderately or severely affected. And as seen in our story about Sam, different teeth can be affected to different degrees in the same mouth – so sometimes the presence of just one or two badly affected teeth can have a big influence over what type of care is recommended for your child.
The way that dental professionals manage Molar Hypomin really depends on how badly your child’s teeth are affected. Of course teeth that are mildly defective require easier treatments than those that are moderately or severely affected. And as seen in our story about Sam, different teeth can be affected to different degrees in the same mouth – so sometimes the presence of just one or two badly affected teeth can have a big influence over what type of care is recommended for your child.
As well as looking at the Molar Hypomin problems, other aspects of oral health will be evaluated including the extent of any dental caries and how well your child’s "bite" (occlusion) fits together. Of course, how old your child is and how well they might cope with complex dental treatment will also be taken into account. Depending on the long-term goals for your child’s well-being and your financial situation, a dental care plan will then be suggested and discussed with you.
Some examples of common treatments used for different grades of Molar Hypomin, and an indication of how challenging kids might find them, are listed below:
MILD CASES

When a tooth is mildly affected by Hypomin, the main goal is to keep the tooth strong and healthy in an effort to prevent future damage – as the adage goes, “an ounce of prevention is better than a pound of cure”.
Desensitising and hardening treatments
Molar Hypomin kids may complain of pain (sensitivity) when they eat hot or cold foods, or while brushing their teeth. Such dental pain can usually be reduced by putting special coatings on the sensitive areas of the tooth, thereby making your child’s life much more pleasant (yours too, probably). Your dentist may also recommend a "desensitising" or "dental hardening" product (toothpaste, gel, foamy cream, or even a medicated chewing gum) for regular use at home, which may further reduce sensitivity and make (all) the teeth harder. You will be told how much to use and how often, depending on your child’s problem.
Fissure sealants
Since Hypomin teeth are often chalky (i.e. softer and more porous than normal), there is increased risk that "bugs" will get in and cause dental caries. If the defective patch is small and not yet "potholed" (i.e. the surface is intact, not broken), the Dental Therapist or Dentist may paint on a protective covering to help keep the bugs out. This treatment, called fissure sealing, is generally simple to perform and relatively inexpensive – the tooth is cleaned and then coated with a paint-like resin (usually coloured white or pink) that is set rapidly using a bright light. Although fissure sealants can be very effective in preventing dental caries, ongoing home care remains a key responsibility for your child and you. It is important to know that, in many cases of Molar Hypomin, fissure sealants don't stick as well as they do to normal teeth – so regular dental check-ups are really important even for kids with just a mild case of Molar Hypomin.
Child management issues
For most kids the treatment of mildly affected teeth is nothing to be concerned about. Generally there is no need for drilling and hence no need for injections and the like. If a really good job is to be done placing fissure sealants then this will require some co-operation from your child – but most take this in their stride quite readily and are happy to help out in making their teeth stronger.
MODERATE CASES

Moderately affected Hypomin teeth are already "potholed" to some extent, putting them at risk of dental caries and further crumbling or "breakdown". A dental filling is usually recommended to stall these problems and, when combined with ongoing home care, can often provide a reasonably long-lasting outcome.
Tooth-coloured fillings
Where a relatively small area of the tooth is defective, a simple type of filling is generally recommended. Usually a "tooth-coloured dental composite" filling is put in, much the same as for a normal tooth. However, as with fissure sealants (see MILD CASES, above), these resin-based fillings may not stick as well they do to normal teeth, necessitating regular check-ups and perhaps more frequent replacement.
Customised onlay fillings
When the patch of broken-down tooth enamel is more extensive, your dentist may recommend a dental onlay which is a very strong filling specially customised for your child. After the defective tooth material has been trimmed away, a mould of the tooth (dental impression) will be sent to a dental technician so that the onlay filling can be made to fit your child’s tooth precisely. A second appointment is needed to glue the onlay to the tooth. This treatment can be quite a bit more expensive because of the extra steps involved and the use of an extra-strong metal filling material.
Child management issues
When your child needs a dental filling some gentle drilling is usually required to remove the crumbly bits of enamel. While not always necessary, often it’s best to numb the tooth first with "a local" (local anaesthetic) – which of course means a small injection of some sort. Dentists have many tricks up their sleeves for avoiding this being an unpleasant experience for your child so generally it’s best for parents not to say much about it – certainly any talk about "the needle" is best avoided since your Dentist will likely want to use well-researched methods that focus on the positive benefits gained from numbing the tooth. Moreover, by first rubbing some "teething gel" (topical anaesthetic) on the gum, most injections can be so painless that your child won’t even register that they’ve "had a needle".
For some kids a troublesome feature of Molar Hypomin is that it can be quite difficult to make their teeth go numb. So it's important to believe them if they complain of some discomfort during dental treatment, even if their face and other teeth are completely numb. And for kids who are a bit more restless than most, a stronger option than local anaesthetic might be a wise choice (e.g. sedation or general anaesthetic) – your Dentist will let you know if these alternatives seem preferable.
While getting regular tooth-coloured fillings is a breeze for most kids, the lengthier procedures needed for custom-made onlays can be more challenging. So onlays are generally restricted to kids who can be 100% cooperative. If your child is anxious or has a short attention span then onlays are probably not the best treatment for them.
SEVERE CASES

When the Molar Hypomin is really severe, it is usual for dentists to ask themselves "are these defective teeth worth saving?". As noted above, your child may be referred to an Orthodontist or Paediatric Dentistry specialist to help you all make this decision wisely. Many factors need to be considered as mentioned elsewhere. But mostly the options will boil down to either covering the tooth with a strong cap (dental crown) or instead taking it out (dental extraction), perhaps along with some other teeth.
Stainless Steel Crowns
When it has been decided to try and save a Hypomin molar that's severely broken down, a Stainless Steel Crown is often regarded as the best treatment. This works as a very strong metal cap that covers the whole tooth and holds it all together – it also helps protect the damaged tooth from dental caries and thermal sensitivity. Because these "silver" crowns are shiny and sparkly, it often helps to tell young kids they're getting “robot teeth” or “princess teeth” (which makes many of them think they're pretty cool). Generally these Stainless Steel Crowns are used as a temporary measure until your child is old enough to undergo the lengthier procedures of making a "permanent" dental crown – these are made out of tooth-coloured porcelain or gold and cost much more.
Extractions and orthodontics
Sometimes it is clear that the best option is to have the defective tooth removed. Often this can be viewed as a beneficial outcome because it means that particular tooth won't cause any more pain or need any more fillings. However, taking just one tooth out may cause an imbalance in your child's bite (occlusion). So this is why an Orthodontist is often consulted about the advisability of doing additional "balancing extractions" – typically the equivalent tooth on the opposite side of the jaw may be taken out too which of course then leaves you with a particularly well-balanced kid (orthodontically at least!).
When a 6-year molar ("first adult molar") is taken out at an appropriate time (typically between 9- and 11-years old) it's possible that the second adult molar (i.e. "12-year molar") will subsequently come up and move forward into its place. However the chances of this working really well are rather iffy so this treatment option needs to be monitored regularly by a Dentist and/or Orthodontist. In turn, if your child has an appropriate "wisdom tooth" (third adult molar) growing inside their jaw, this may eventually erupt and move into the place of the 12-year molar – but again this is hard to predict. If the teeth do not eventually work their way into a good bite, the services of an Orthodontist may be needed (read more about orthodontic braces). Of course many Molar Hypomin kids have other reasons to visit the Orthodontist, and many kids without Molar Hypomin have extractions as part of their orthodontic treatment, so it's important not to feel overly nervous if this option is being discussed for your child.
Treatment for incisors
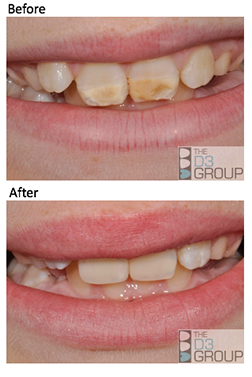
When the front teeth (incisors) are also affected, as sometimes happens in severe cases of Molar Hypomin, the main concerns usually relate to an unappealing appearance – this can be disconcerting for family and friends, not just the affected child. Most often a good appearance can be restored simply by use of tooth-coloured fillings (see MODERATE CASES, above) as the picture shows for our 10-year-old friend from our Molar Hypomin page. Sometimes dental bleaching might also be used, to reduce any strong discolouration.
Child management issues
For many kids and especially the younger ones, placement of Stainless Steel Crowns and the extraction of teeth can be a bit too much to cope with comfortably – and of course this has repercussions for Dentists trying to do a "good fix" and for loving parents who may be watching. In these cases excellent alternatives exist (sedation and general anaesthesia) and are often recommended as the best path to take – a prime reason being that they allow more, if not all, treatment to be performed in one go, so minimising anxiety for all concerned.